 Diabetes is reaching near epidemic proportions world-wide. In the United States, the prevalence of Diabetes has increased by 45% in the past 20 years and the CDC warns that if the current trend continues, 1 in 3 Americans will be afflicted with this potentially fatal condition by 2050. Diabetic eye disease is the leading cause of new blindness in the United States for patients between the ages of 25-65 and with the explosion of new diabetes diagnosis; this unfortunate trend is likely to continue.
Diabetes is reaching near epidemic proportions world-wide. In the United States, the prevalence of Diabetes has increased by 45% in the past 20 years and the CDC warns that if the current trend continues, 1 in 3 Americans will be afflicted with this potentially fatal condition by 2050. Diabetic eye disease is the leading cause of new blindness in the United States for patients between the ages of 25-65 and with the explosion of new diabetes diagnosis; this unfortunate trend is likely to continue.
Diabetes is a vascular disease that occurs when blood glucose levels are inadequately controlled by the body’s internal regulatory mechanisms which results in increased glucose, or sugar, in the blood. There are several different forms of diabetes but the main two are types 1 and 2.
• Type 1 Diabetes or juvenile onset diabetes represents about 10-15% of all diabetics in the US and occurs when the pancreas, the organ that produces insulin, is attacked by a person’s own antibodies. Insulin is important because it allows the human body to clear glucose out of the blood and use it for energy. The autoimmune damage to this organ and loss of the insulin producing cells is why Type 1 Diabetics are typically diagnosed earlier in life and require lifelong supplemental insulin.
• Type 2 Diabetes is very different. With this condition there is plenty of insulin being created, however, the body over time becomes resistant to its effects. Treatment for this type of Diabetes includes diet and exercise, oral medications, and insulin injections.
Regardless of the type, if glucose is allowed to build up in the blood, the walls of the blood vessels begin to become damaged which prevents proper circulation and can cause the blood vessels to become weak to the point where they hemorrhage, leak, or become clogged. It is this underlying cause that results in damage to the eye as well as the kidneys and circulation to the hands and feet.
Read more about Diabetes:
http://www.diabetes.org/
http://www.nlm.nih.gov/medlineplus/diabetes.html
Diabetic Eye Disease and Retinopathy
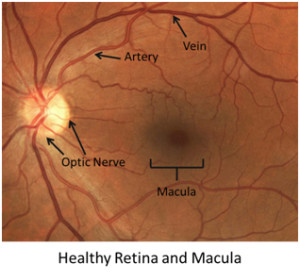
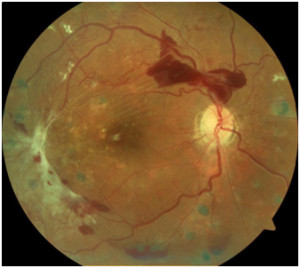 Diabetic eye disease is the leading cause of blindness in the United States from the ages of 25-65. All people who have diabetes, regardless of the type or severity, are at risk for developing diabetic eye disease. There is a thin tissue lining the inside of our eye called the retina. When you look at an object, the light rays in your surroundings bounces off the object and move toward your eye. The light rays pass through various structures of your eye and are focused on the retina which captures the light like film in a camera. The retina has a vast network of very small, delicate blood vessels that can be susceptible to damage caused by diabetes. When the blood vessels of the retina are damaged by diabetes, they can begin to leak which causes swelling and damage to this sensitive tissue, this is referred to as Diabetic Retinopathy. In addition to leaking, continued damage causes the vessels to clog and parts of the retina become oxygen starved from lack of blood. This hypoxia, or lack of oxygen, causes the starving tissues to release chemicals that cause new blood vessel growth. This is a severe consequence of diabetic retinopathy because the new blood vessels are prone to leaking, scarring, and hemorrhaging into the jelly of the eye, called the vitreous. The scarring can also cause traction or pulling on the retina leading to retinal detachments.
Diabetic eye disease is the leading cause of blindness in the United States from the ages of 25-65. All people who have diabetes, regardless of the type or severity, are at risk for developing diabetic eye disease. There is a thin tissue lining the inside of our eye called the retina. When you look at an object, the light rays in your surroundings bounces off the object and move toward your eye. The light rays pass through various structures of your eye and are focused on the retina which captures the light like film in a camera. The retina has a vast network of very small, delicate blood vessels that can be susceptible to damage caused by diabetes. When the blood vessels of the retina are damaged by diabetes, they can begin to leak which causes swelling and damage to this sensitive tissue, this is referred to as Diabetic Retinopathy. In addition to leaking, continued damage causes the vessels to clog and parts of the retina become oxygen starved from lack of blood. This hypoxia, or lack of oxygen, causes the starving tissues to release chemicals that cause new blood vessel growth. This is a severe consequence of diabetic retinopathy because the new blood vessels are prone to leaking, scarring, and hemorrhaging into the jelly of the eye, called the vitreous. The scarring can also cause traction or pulling on the retina leading to retinal detachments.
Read more about Diabetic Retinopathy:
http://www.nei.nih.gov/health/diabetic/retinopathy.asp
http://www.nlm.nih.gov/medlineplus/diabeticeyeproblems.html
Diabetic Macular Edema
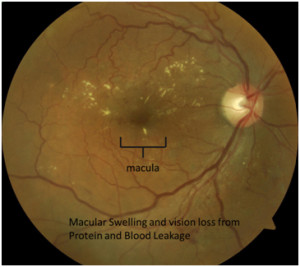 The area in the center of the retina is called the macula. Also involved in macular degeneration, the macula is responsible for your central vision, your ability to see fine detail, and your ability to see colors. If the blood vessels in the area of the macula are damaged by diabetes, they can begin to leak. The leaking of blood and protein rich fluid from the blood vessels in this area can lead to swelling of the macula which results in decreased and distorted vision. If the macula is short circuited from the swelling for long periods, the visual reduction can be permanent.
The area in the center of the retina is called the macula. Also involved in macular degeneration, the macula is responsible for your central vision, your ability to see fine detail, and your ability to see colors. If the blood vessels in the area of the macula are damaged by diabetes, they can begin to leak. The leaking of blood and protein rich fluid from the blood vessels in this area can lead to swelling of the macula which results in decreased and distorted vision. If the macula is short circuited from the swelling for long periods, the visual reduction can be permanent.
Read more about Diabetic Macular Edema:
http://www.bausch.com/eye-concerns/eye-diseases-and-disorders/diabetic-macular-edema-dme/
http://www.nei.nih.gov/health/diabetic/retinopathy.asp
Treatment of Diabetic Retinopathy and Macular Edema
Treatment options for diabetic retinopathy range from observation to surgery, depending on the severity of the disease. In most cases of diabetic retinopathy, simple observation with a higher frequency will be recommended by your eye doctor. If further changes are noted that could potentially cause vision loss, ocular surgery under the care of a retinal specialist may be recommended.
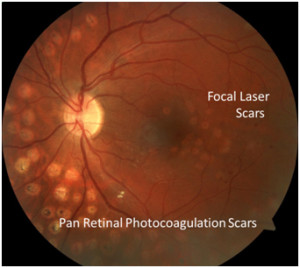
Common Treatment for macula edema comes in the form of low energy focal laser near the macula to close off the leaking blood vessels and reduce swelling. If diabetic retinopathy gets severe enough that a large portion of the retina is not getting blood or new blood vessels begin growing, Pan Retinal Photocoagulation or PRP is often performed to prevent or stop new blood vessel growth. With either severe retinopathy or macula edema, eye injections are also very effective at preserving vision.
Cranial Nerve Palsies from Diabetic Eye Disease
We have 12 cranial nerves that course throughout various parts of our brain. Of these 12 cranial nerves, four are responsible for the proper function of our eyes. If diabetes causes damage to the blood vessels that supply these cranial nerves, they can become dysfunctional and impair vision. Cranial nerves 3, 4, and 6 control eye position and movement. If one (or more) of these nerves is affected by diabetes, the result can be an eye that turns in, out, up, or down. When the eyes are not pointed in the same direction, double vision can result.
Treatment of Cranial Nerve Palsies
Cranial nerve palsies that are caused by decreased blood flow to the nerve secondary to diabetes usually resolve without intervention over the course of several weeks. Treatment is aimed at alleviating the visual symptoms (often double vision) until the function of the nerve is restored. This can be done by either patching the affected eye or by the use of special corrective lenses that use prism to improve the double vision. Cranial nerve palsies caused by improper blood flow to the nerve secondary to diabetes may be a diagnosis of exclusion, meaning that your doctor may order other tests to rule out more serious causes. In some cases, the double vision may be permanent, and require long term use of prism-containing spectacle lenses.
Read more about Cranial Nerve Palsies:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2801485/
http://faculty.washington.edu/chudler/cranial.html
http://www.patient.co.uk/doctor/Diplopia-and-Cranial-Nerve-Lesions.htm
Neovascular Glaucoma from Diabetic Eye Disease
Our eyes receive oxygen from blood, and if diabetes does enough damage to the blood vessels in the eye, a lack of oxygen supply can result. Sometimes, this can stimulate the eye to begin to build new blood vessels. It sounds like a novel attempt, but in reality, these blood vessels are structurally weak and function very poorly. These vessels often form on the retina but if the diabetic eye disease is severe enough, the new blood vessels can form on the iris at the front of the eye. Here the new forming blood vessels can severely restrict the eye’s drainage system which results in a very severe and often painful form of glaucoma called neovascular glaucoma.
Treatment of Neovascular Glaucoma
Treatment of Neovascular Glaucoma is aimed at decreasing the oxygen demand of the eye by using a laser (PRP laser) to exterminate areas of the retina that are not getting enough blood. This provides a situation where there is less living tissue, requiring less oxygen and thereby eliminating the eye’s perceived “need” for building new blood vessels. Another treatment option is the injection of a drug that inhibits the production and growth of the new, faulty blood vessels.